Changes to BC’s COVID-19 Long-Term Care Visitor Policy
August 28, 2020
BY Sara Pon
Introduction
On June 30, 2020 the BC government announced that the visitor policy for long-term care and assisted living would be changing. In the new policy residents can have one designated visitor for social visits. Prior to this policy change, only essential visitors were allowed in long-term care and assisted living (discussed below). This new policy can take effect as soon as individual facilities have plans in place and have implemented the changes required. As of August 6, all 563 long-term care and assisted living facilities in the province have safety plans in place, although some of these facilities are in outbreak status and not currently accepting visitors.
Family/Social Visits
Under the new policy, visitors will be allowed into long-term care and assisted living for social visits. Each resident will designate a specific person who will be allowed to visit them. Under the current policy, the resident will only be allowed to visit with this designated person, and the designated person cannot be changed. These visits are intended to provide social and emotional support, not to provide medical or personal care.
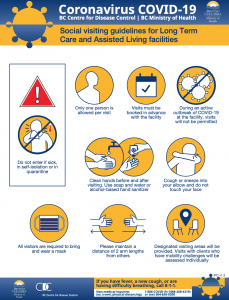
The following procedures must be followed for arranging family/social visits:
- Only the designated family or friend may visit
- Visits must be scheduled in advance with the facility
- Visitors will be informed of the procedures and guidelines in advance
- Visitors will be screened for symptoms of illness prior to the visit
- The facility must post signage on visit and infection control procedures
The following procedures must be followed during the visit:
- Staff members will oversee visits to ensure procedures are being followed
- Visitors can only enter the facility if they have no signs of illness and they are not in self-isolation or quarantine
- Visitors will be instructed by staff on how to wash their hands, how to put on a mask and other required PPE, and how to keep a safe physical distance
- Visitors must wear masks
- Visitors must clean their hands upon entry and exit
- Visitors must sign in upon entry
- Visits must occur in the designated area
- Visitors must go directly to the designated area, and directly out of the facility
- Visitors must keep a safe physical distance from residents, and not engage in any physical contact such as hugging
Family /social visits will be suspended if a COVID-19 outbreak occurs at the facility. An outbreak occurs when at least one resident or staff member tests positive for COVID-19. Visits can resume once the outbreak has ended. An outbreak is considered over when two full incubation periods have occurred (28 days) since the last exposure.
For visits outside of the facility, the policy differentiates between long-term care and assisted living. For long-term care, the guidance advises residents to only leave the facility for medically necessary reasons. For assisted living, the guidance allows residents to have social and other activities outside the assisted living facility, provided they are complying with general public health guidance. This would mean residents would be able to visit other people who are not their designated visitors outside of the facility, as long as they are physically distancing.
Essential Visits
Essential visits are continuing under the new policy. Visitors can enter the facility for a variety of reasons, including:
- End-of-life care;
- Visits necessary for physical care or well-being;
- Communication assistance; and
- Supported decision-making.
The resident is allowed one visitor at a time, except for end-of-life care when more visitors are permitted at the same time. Facility staff or health authorities determine what visits are essential. If a visitor is denied entry because their visit is deemed non-essential, they can request a review from a facility administrator or the Patient Care Quality Office.
Essential visits are still allowed when a facility has a COVID-19 outbreak. Essential visitors must wear masks and keep physically distanced. If the resident is infected, the visitor is to be given PPE under the PPE Allocation Framework.
Personal Services
Under the new policy, personal services will now be allowed in long-term care and assisted living, including hairdressing. All personal service providers must follow the WorkSafeBC protocols, including wearing masks and using correct hand hygiene protocols. Before personal service providers can enter the facility, they must get their safety plans approved by the facility operator. Operators must keep a list of all residents who use personal services and when this service occurred.
Facility Implementation
Before visits can resume, facilities must have a plan in place for how they are going to implement this policy. When developing their implementation plans, the operators must work with residents, families, and care providers.
Each facility must determine where their designated visiting areas will be. There should be an outdoor location where visits can occur when the weather permits, and indoor designated locations. Additionally, visits can occur in a client’s room if the room is single-occupancy and the resident does not have the mobility to go to the designated visiting area. The specific location and number of visiting locations will depend on the size of the facility. Each facility must determine where their designated visiting locations will be.
Facilities must determine how many visitors they can accommodate per day, how long the visits can last, and how many visits per month a visitor can make. The facilities must set these policies because the number and length of visits will be determined by the size of the facility and how many designated visitor areas they can fit into their facility. If the facility has room for multiple visitor rooms, they may be able to accommodate more visitors per day than a small facility.
Once facilities create their plan, they must post the details about visit locations and procedures on their websites and inform residents and families in writing. Signage must be put up stating the facility visiting policies and showing the precautions that must be taken, such as wearing masks and handwashing.
Facilities must sanitize furniture and surfaces in the visiting areas between all visits. Facilities must schedule visits so there is enough time in between visits to complete this sanitization. Facilities must keep a record with contact information of all visitors into the facility for contract tracing purposes.
Funding for Additional Staff
This new visitor policy will require staff be available for organizing and monitoring the new visits. The Ministry of Health is providing funding for each facility to hire three full-time equivalent staff responsible for infection prevention and control measures for visits. This money is being provided to both public and private facilities.
Review of the Current Policy
Each facility must conduct monthly reviews of their policies and practices to ensure they are following the new guidance. The Ministry of Health stated during the press conference that they will monitor the new policy and will consider changes to the policy. Changes to the policy could include increasing the number of designated visitors and change to how visits are conducted.
Health Care Laws in BC
It is important to keep in mind the rights of residents, which do not change during the COVID-19 pandemic. In BC, the Health Care (Consent) and Care Facility (Admission) Act states that all adults have the right to have a supporter help them make decisions. This right exists whether or not a person has designated a representative under a Representation Agreement. Under section 16 of the HCCA, if the adult does not have capacity for health care decisions, the health care provider must make reasonable efforts to obtain consent from the appropriate substitute decision-maker before providing medical care. This could be a representative under a Representation Agreement, a committee or personal guardian, or a temporary substitute decision-maker. The substitute decision-maker must consult with the person they represent, which may necessitate in-person contact.
Under the COVID-19 guidance for long-term care and assisted living, visits for supported decision-making and communication assistance are considered essential. Supported or substitute decision-makers should be allowed in under the essential visit category. If the supported or substitute decision-maker is not allowed into the facility to help make these decisions, this can be appealed. The policy to consider supported decision-making essential aligns with the right to supported decision-making in BC.
The Community Care and Assisted Living Act sets out the residents’ Bill of Rights. These include the right to have visitors, to communicate with their visitors in private, and to have their family be involved in their care plans. Under the new COVID-19 guidance, allowing a visitor is an important step to fulfilling the resident’s right to have a visitor. The degree to which these visits are private may depend on the specific facility and on how private the designated visitor area is. How frequently the resident will be able to visit with their designated person will depend on the facility. A resident will not be able to visit with anyone if their designated visitor is sick, because the resident can only have one designated person.
Resources
- To view the entire policy, see the BC CDC website.
- For more information on health care decision-making rights, see the CCEL’s decision-making resources.
- Alzheimer Society of B.C has created a resource to help people prepare for visits to long-term care.
Click on the poster to enlarge